Nerves are formed by the axons of nerve cells (the axon is an extension of the nerve cell). These axons are or are not surrounded by myelin sheath from other cells: Schawnn cells.
Anatomy:
A nerve is made up of different elements:
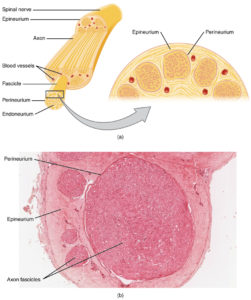
- Axon
The axon is a nerve fiber that originates from the cell body of the neuron and varies in length depending on the cell from 1mm to over 1m. The axons, when they travel, at the periphery but also in the CNS, are most often grouped into bundles, called fascicles. The axons follow an undulating path in the fascicles, which gives them the ability to lengthen during the various joint movements. An axon carries an action potential between the cell body and another nerve, gland, receptor, or motor (muscle) unit. The axon also carries different molecules. An axon can have collateral branches, which emanate from the main axon. The end of the axons is called synaptic button. A synapse is where synaptic knobs interact with the plasma membrane of another neuron or cell.
The cytoplasm of an axon is called axoplasm and the plasma membrane is called axolemma. The axon may be covered with a lamellar layer of myelin which forms an outer sheath called the myelin sheath. A nerve fiber with a myelin sheath is called a myelinated fiber; a nerve fiber that lacks a myelin sheath is called an unmyelinated fiber. The myelin sheath cells for the peripheral nervous system is Schwann cell. The innermost layer of the Schwann cell is the neurolemma (Greek: neuro, nerve; lemma, envelope). The myelin sheath is classically interrupted at regular intervals by depressions called neuro-fibrous nodes or, more colloquially, nodes of Ranvier. The distance between the nodes is the inter-nodal distance. Myelin is absent at each node. The myelin envelope increases the speed of conduction of nerve impulses. Myelinated nerves transmit nerve impulses at speeds between 3 m/s and 120 m/s; unmyelinated fibers confer speeds of 0.7 to 2.3 m/s
- Endoneurium
The endoneurium is the innermost or deepest layer of connective tissue comprised within a peripheral nerve. It forms an interstitial layer around each fiber outside the neurolemma. This very cohesive connective tissue matrix also contains capillaries, mast cells, Schwann cells and fibroblasts.
- Perineurium
Each fascicle is surrounded by a sheath, the perineurium. The perineurium has three main functions:
-
- Protect the endoneurial tubes from the tensile and compressive forces applied to it by body movements, thanks to its collagen and elastin fibers.
- Protect the endoneurial tube from external trauma.
- Constitutes a barrier against various chemical aggressions (neurotoxic) via a blood-nervous barrier.
Epineurium
- Epineurium is a loose connective tissue, is subdivided into two layers, internal and external. The inner epineurium constitutes the basic collagenous tissue that physically separates the fascicles. It performs two basic functions:
- the outer layer provides protection of the nerve trunk against compressive forces and, more importantly, to facilitate sliding between the fascicles. This epineurium is particularly present within the nerve segments which are confronted with compression-sliding forces next to nerve tunnels (cubital tunnel; carpal tunnel; tarsal canal,).
- The external epineurium surrounds the nerve trunk and provides protection against compressive and tensile forces.
mesonevre
- The mesoneurium is the outermost tissue surrounding the peripheral nerve trunks. It is a loose, areolar tissue that carries many arteries and veins that supply the nervous tissue: the vasa nervorum.
Nerves can be classified according to their size:
Name Diameter Conduction Velocity Role
A alpha 13-30 µm 80-120 m/s Proprioception (motor skills)
A béta 6-12 µm 35-75 m/s Sensitivity
A delta 1-5 µm 5-35 m/s Pain. Temperature
C 0,2-1,5 µm 0,5-2 m/s Pain. Temperature
The A alpha, A beta and A delta fibers or nerves have a myelin sheath, the C fibers do not.
They can be classified by their functions:
Efferent fibers carry information from the center to the periphery.
Afferent fibers carry information from the periphery to the center.
Efferent fibers are composed of:
- Somatic motor nerves that innervate the striate musculature (motor muscle).
The striated muscle is the muscle of movement: the biceps, for example, which allows you to bend your arm or the calf which allows you to stand on tiptoe or press the pedal of the bicycle. - Nerves of the vegetative system which innervate the smooth muscles (in particular in the intestines), the heart and certain glands.
Afferent fibers carry sensory information. They are composed of:
- Myelinated fibers for tactile sensitivity (touch), proprioceptive (position of a joint, length of a muscle), some painful and thermal information.
- Unmyelinated fibers for pain and temperature.
Afferent fibers carry information from more or less specialized receptors:
- Sensory receptors: mechanoceptors sensitive to pressure (corpuscles of Pacini, Ruffini, Meissner, Merkel cells) and the stretching of the skin, chemoreceptors for taste and olfaction and finally teleceptors for vision,
- Proprioceptors: measures pressure and tension in muscles, joints and tendons (Golgi tendon organ, Pacini corpuscle, Ruffini corpuscle),
- Interoceptors: modified by modifications of the internal environment (baroreceptors, chemoreceptors)
- Nociceptors: polymodal (several types of stimuli) or specific.
The vegetative system is composed of the orthosympathetic system and the parasympathetic system. these two systems are, in general, antagonists and take care of the innervation of the deep organs (heart, stomach, intestine, sweat of the skin,…)
Composition of a nerve:
The afferent and efferent fibers join to form mixed (sensitivomotor) nerves, sciatic nerve for example.
The efferent fibers alone form a motor nerve (facial nerve for example).
The afferent fibers alone form a sensory nerve (trigeminal nerve for example).
Pathology: Peripheral neuropathies.
The different attacks are described according to whether or not the axon is affected, whether or not the myelin sheath is affected,
The achievement of an efferent nerve gives paralysis or paresis.
Involvement of an afferent nerve leads to disturbances in superficial (touch) and/or deep (proprioception) sensitivity.
Involvement of the autonomic nervous system gives rise to a dysautonomic syndrome.
Isolated involvement of small A delta and C fibers results in small fiber neuropathy.
Functional exploration: Electrofisiological examinations.
The nerve has the property of conducting nerve impulses. The application of an electric current to its level causes the formation of an action potential. Collecting the nerve potential (sum of the action potentials) at a distance from the stimulation is the basis of the technique for measuring motor and/or sensory conduction velocities.
Motor conduction is measured after stimulation at the level of the muscles, it is the motor response.
Sensory conduction is measured by stimulating the nerve and collecting a nerve potential (sum of nerve action potentials).
These are sometimes unpleasant or even painful, patients should be warned.
The different exams available are:
- Electromyogram by nerve stimulation and also collection of spontaneous or voluntary muscle activity.
- Somatosensory evoked potentials by cutaneous stimulation with collection of the response remotely along the path of the nerve or at the level of the skull.
- Motor evoked potentials by transcranial magnetic stimulation at the level of the motor cortex and collection of the response at the muscular level.
These different examinations make it possible to define neurological damage by differentiating between damage to the axon (axonopathies) or myelin (myelinopathies).
Axonopathies
In the event of an acute attack, for example a trauma, there are 3 stages of nerve damage:
- Neupraxia corresponds to an isolated impairment of the myelin sheath,
- Axonotmesis corresponds to an axonal attack without interruption of continuity,
- Neurotmesis corresponds to the rupture of continuity of the nerve.
In the case of chronic damage, there is little slowing down of nerve conduction velocity but a reduction in amplitude by reduction in the number of functional axons. This reduction is length dependent: the further away from the central nervous system the greater the loss (see small fiber neuropathy and acute polyradiculoneuritis development).
Myelinopathies
The disappearance or impairment of the myelin sheath leads to a marked decrease in conduction velocities during electrophysiological examinations.
