This article is heavily inspired by the book “Explain Pain Supercharger” written by G. Lorimer Moseley and Davis S. Butler
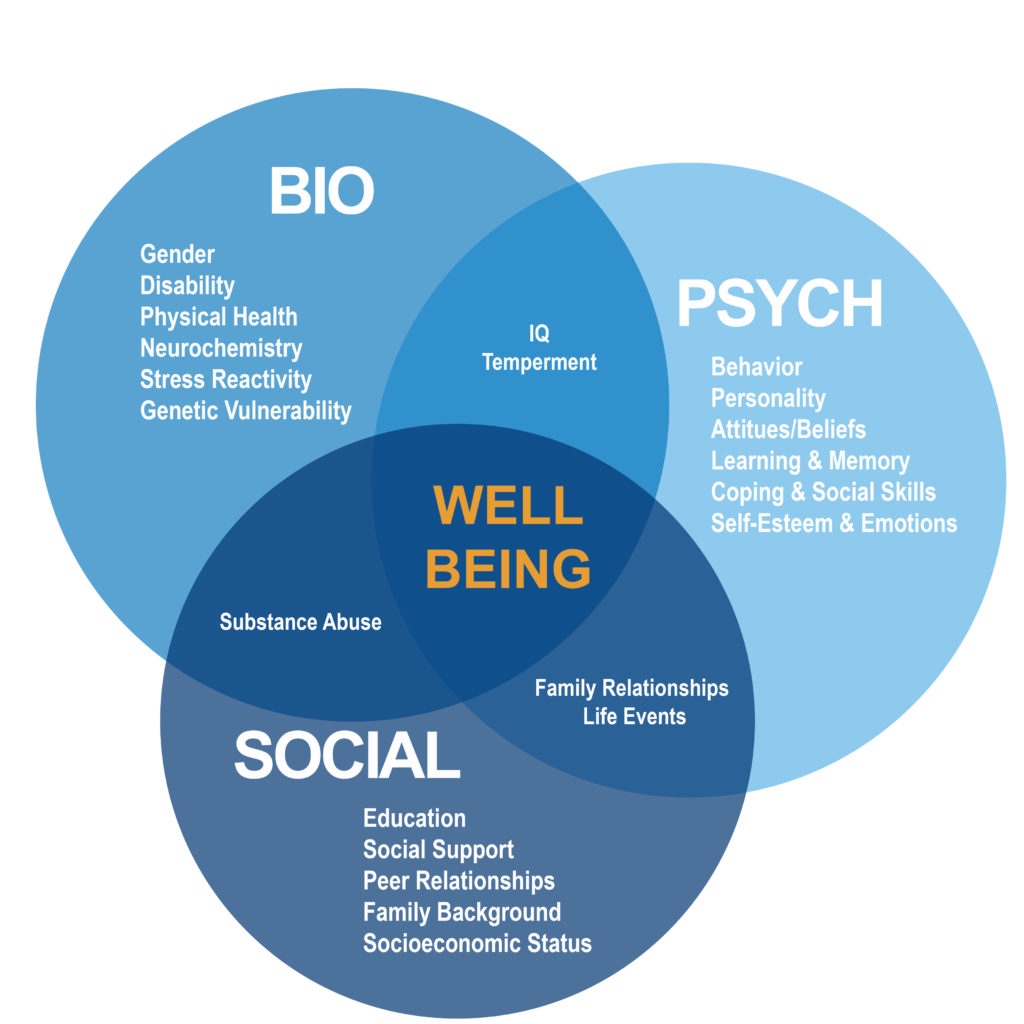
The biopsychosocial model to explain chronic pain
This model takes into account the individual as a whole to explain his state of health and therefore also the problem of chronic pain. It is described by the following diagram (items in blue are not exhaustive):
Pain and nociception: they are not the same
Definition of pain: it is an unpleasant sensation and emotional experience in response to actual or potential tissue damage or described in these terms
Definition of nociception: Nociception is the set of processes making it possible to encode, transmit and process the nervous message from nociceptors.
The definition of nociceptors is complex: it is a receptor which will, under certain conditions, send electrical signals to the central nervous system indicating an anomaly which must be considered as dangerous, lesional or pre-lesional:
- polymodal receptors (free endings responding to various stimuli)
- mechanoreceptors (deformation, pressure)
- chemoreceptors (chemical modification)
- Thermoreceptors (temperature)
There are specific receptors that respond to intense stimulation (hot, cold, deformations, etc.) and sensory receptors that, under certain conditions, will send a nociceptive message.
The usual sensory receptors can be sensitized by local inflammation, or by changes in the central nervous system.
The difference between pain and nociception is important
- Pain is always felt in a living being, nociception can be triggered on a cell in the laboratory
- Pain is felt somewhere, nociception happens somewhere (it doesn’t have to be the same place)
- Pain is felt, nociception is not.
- A nociceptive message does not necessarily cause pain and conversely a sensory message can cause pain.
Nociceptive message modulation concept
- The modification of local conditions by lesional or neurogenic inflammatory processes (of nervous origin) modify the response of local nociceptors and receptors to stimuli.
- There is a medullary sensitization process capable of modifying the nociceptive or sensory message
- There is a central sensitization process capable of modifying the nociceptive message at all levels in a direct way (inhibitory control or top-down facilitator, hormonal system, immune system,…). Which brings us back to biopsychosocial models.
Chronic pain
Definition: after 3 to 6 months, persistent pain that resists the usual treatments is said to be chronic.
Chronic pain theory
- Pain is a protector and not an information.
- Pain exists in relation to future events, not past ones.
- She’s trying to keep you safe.
- It appears when the various elements of the nervous system (which function like a matrix) are more in favor of the existence of a danger for you than of a feeling of security for you ( Moseley GL and Butler DS. 2015. The explain pain handbook: Protectometer. Noigroup Publications: Adelaide.).
The elements that are in favor of a danger are DIMs and the elements rather in favor of safety are SIMs. The DIMs and the SIMs are modulated by “neurotags” which are elements of the neural network which will modify the DIMs and the SIMs in one direction or the other. The treatment of chronic pain will focus on modifying or creating neurotags in order to reduce the DIM and strengthen the SIM. There are two types of neurotags: those that exert an action beyond the brain (muscles, nerves, state of consciousness, etc.) and those that exert a solely central action (knowledge, feelings, etc.). (Wallwork SB et al.(2015). Neural representations and the cortical body matrix : implications for sports medicine and futur directions. Br J Sports Med. Dec 2015. doi : 10.1136/bjsports-2015-095356.).
These different elements lead us to a dozen concepts explained in “Explain pain supercharged by G. Lorimer Moseley and David S. Butler 2017. p 128. Edition Noigroup.”
- Pain is normal, personal and always real. Pain is a normal experience and is an excellent, if unpleasant, response to what your brain considers a dangerous situation.
- There are danger sensors, not pain sensors. The danger alarm system is just that. There is no pain sensor, pain pathway or pain target.
- Pain and tissue damage are rarely completely linked. Pain is not a reliable indicator of the presence and extent of tissue damage. One can exist without the other.
- Pain depends on the balance between danger and safety. You will be hurt if your brain concludes that there is a situation that is obviously more dangerous than safe for yourself, it deduces the need to protect yourself.
- Pain leads to diffuse brain activity. There is no pain center in the brain. Pain is a conscious sensory experience that involves many areas of the brain over time.
- Pain depends on the context. Pain can be influenced by things you see, smell, hear, taste or touch, things you say or believe, things you do or places you visit or people you meet or know. and finally by what you feel in your body.
- Pain is one defense system among others. When threatened, the body is able to activate multiple protective systems: the immune, endocrine, motor, autonomic nervous, respiratory, cognitive, emotional and pain systems. Any of these systems can become oversized and therefore unsuitable.
- We are bioplastic. While all systems can be activated and excited, the notion of bioplasticity suggests that they can go back, during life. It is biologically impossible to think that pain cannot change.
Learning how pain works can help individuals and society. Learning how pain works is therapy. When you understand why you suffer, you suffer less (Mosely GL (2009) Explaining pain to patients- recent developments. Proceedings of the New Zealand Pain Society. Annual scientific meeting.). If you have a pain problem, you are not alone, millions of people have one too. But there are plenty of researchers and clinicians working to find out how you can help. - Active therapeutic strategies promote healing. Once you understand your pain, you can start managing it, exploring different ways to move, improving your physical abilities, eating better, sleeping better, breaking DIMs, finding SIMs, and gradually doing more.
Management of chronic pain
(This part of the article does not come from the aforementioned authors)
Once we have talked about all this information on chronic pain we can begin to see what can be put in place in the treatment of chronic pain, indeed different “modulatory” entry points can thus be put implemented. These modulations can affect:
Afferents (sensory, nociceptive motor)
- Physiotherapy: different treatments are possible and not exclusive. Strengthening, massage, passive or active stretching, Ktape, dermoneuromodulation, etc…
- Osteopathy
- Discharge (immobilization, stop of support of a member)
- Treatment of local inflammation (local or general route)
- Cryotherapy
- Local anesthesia
- Locoregional anesthesia (anesthesia of all or part of a limb)
Unconscious integration of pain
- Drug treatment (analgesics, antiepileptics, antidepressants)
- Cutaneous neurostimulation (by sticking electrodes on the skin), auricular (by an electrode applied in the auditory canal of the left ear)
- Spinal cord neurostimulation (by electrodes placed in the spine capable of stimulating the spinal cord opposite)
- Transcranial magnetic neurostimulation (use of a coil on the surface of the skull capable of stimulating the cerebral cortex)(under evaluation)
- Magnetotherapy (30 to 40 minute treatment on a mat sending magnetic waves)
Conscious integration of pain
- Hypnosis
- Mental imagery
- Mindful meditation
Perception of the body
- Mirror therapy
- Vestibular stimulation
- Virtual reality (under evaluation)
Behaviour
- Cognitive-behavioral therapy
- EMDR (Eye movement desensitization and reprocessing)
Comments
This list of support techniques is obviously not exhaustive. But we can already draw some comments:
- The management of chronic pain is complex and therefore requires multidisciplinary care. This care to be consistent is best managed by an algologist doctor who must become the “conductor” of this care
- The various techniques described are for the most part not financially supported by social security systems and mutual health insurance. Chronic pain patients are often financially uncomfortable due to their pathology. The budgets allocated to these treatments must therefore be aligned with the cost of intervention of the various practitioners of these techniques.
- Many answers on the physiopathology of chronic pain are still lacking, an intensification of clinical and basic research is necessary to improve the management of many chronic pain pathologies which will ultimately make it possible to specify the most suitable techniques for each. patient, to shorten care, to reduce the human and social cost of these pathologies.
Dr Yves Guenard